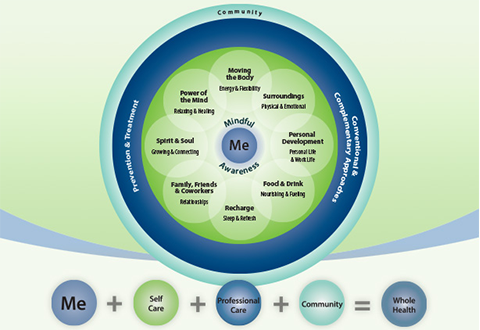
What is Whole Health?
Whole Health is VA’s approach to care that supports your health and well-being. Whole Health centers around what matters to you, not what is the matter with you. This means your health team will get to know you as a person, before working with you to develop a personalized health plan based on your values, needs, and goals.
Learn About How Whole Health Supports Your VA Health Care
How to Get Started
Start a conversation with your VA health team about Whole Health. Use this Brief Personal Health Inventory to start and guide the discussion of your hopes, desires, and goals.
VA staff and Veteran peers can also support you on your Whole Health journey too. Learn about Whole Health practices from other Veterans through the Introduction to Whole Health and Taking Charge of My Life and Health courses. Find the Whole Health contact at your VA here: Whole Health Facility Contacts.
Learn more about getting started with the Personal Health Inventory self-assessment, and Personal Health Plan and how it can shape your Well-being programs and clinical treatments.
The road to better health and well-being starts here, with you.
Start Your Journey With Whole Health Today
Veteran Resources

Whole Health Basics
These resources will help you as you start your Whole Health journey and develop your Personal Health Plan.
Additional Veteran Resources
Whole Health Success Stories
#LiveWholeHealth Series at VA News
Find out how you can practice self-care from home through the #LiveWholeHealth videos. This series highlights Whole Health resources—such as video sessions for yoga or meditation—that you can follow along at home to live healthier and happier.