Office of Health Equity
Addressing Unconscious Biases to Advance Veteran Health Equity
|
 |
Download PDF
INTRODUCTION
Equitable access to high-quality care for all Veterans is a major tenet of the VA health care mission, and the Office of Health Equity (OHE) champions the elimination of health disparities to achieve health equity for all Veterans.
VA health care providers support the Veterans Health Administration’s (VHA) mission, and believe it is both the VA’s and their own personal responsibility to reduce health disparities among patients. Acknowledgement of and actively working to reduce unconscious biases is an essential part of advancing health equity for all patients.
IDENTIFYING UNCONSCIOUS BIAS
Also known as implicit bias, unconscious bias refers to a person's automatic attitudes about others. These biases can shape an individual’s behavior towards others, especially towards people who may be of a different race/ethnicity, gender, sexual orientation, socioeconomic status, disability status, or age.
Unconscious biases are unintentional and common, even in health care. Just as the social context of a patient’s daily living can have an impact on their health, interactions with unconscious bias can also influence their wellbeing or result in poor health outcomes or experiences.
One method then to mitigate unconscious bias in health care settings is partnership building between the patient and provider. Encouraging the patient to view their relationship with their provider as one of “collaborating equals” can give them agency and empower them to have greater say in their treatment plans to improve their health and wellbeing, as well as give them individualism for their providers.
ADDRESSING UNCONSCIOUS BIAS
VA is working hard to ensure that VA health care providers are able to recognize and address any unconscious biases that may influence their interactions with patients. The Office of Health Equity (OHE) provides several online trainings on unconscious bias, as well as other topics centered on cultural competence.
Additionally, OHE partnered with the VA Employee Education System to create a video series on how unconscious bias impacts everyone in the clinical setting. In these short videos, VHA providers share their stories on recognizing and acknowledging their unconscious biases in their clinical practice.
LOCAL EFFORTS
several VA facilities are currently working to address unconscious bias and its consequences. At the Roseburg VA Healthcare System in Oregon established a dedicated workforce to educate VA staff by using a multi-faceted approach on the effects of unconscious bias. Their aim is to illustrate how unconscious thought patterns can influence human behaviors and reactions, and how it impacts patient communication, treatment plans, and team dynamics.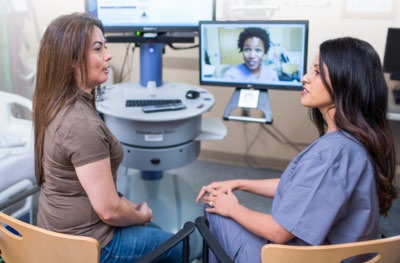
The team at Roseburg places emphasis on being human-connected, individualized, and patient centered. They are hosting workshops for VA staff where they can learn how to better understand the Veteran’s unique experience and wellness goals by personally connecting to the Veteran’s individual health goals, honoring their stories to more fully partner with their Veteran patients, and provide appropriate, high quality care.
Additionally, the VA Boston Healthcare System in Massachusetts, three VA facilities are piloting the introduction of a health-related social needs screening tool, ACORN (Assessing Circumstances and Offering Resources for Needs). ACORN helps health care providers engage in conversations with Veterans around their specific social needs through screening in clinical settings, as well as encourage action planning with providing resource guides to address their areas of need.
The incorporation of social needs screening tools, like the ACORN screener, gives health care providers the opportunity to gain valuable insight about how factors outside their patient’s medical care, like their ability to purchase healthy food, employment stability, or access to reliable transportation, may be impacting their health. This information can help health care providers understand the unique contexts of each Veteran patient to build a more informed relationship with their Veteran patients, and provide targeted, accessible resources to help them be the healthiest versions of themselves.
The Office of Health Equity’s online trainings on unconscious bias and cultural competence trainings can be found at: https://www.va.gov/HEALTHEQUITY/Social_Determinants_of_Health.asp#workforce
For more information about the Office of Health Equity visit: https://www.va.gov/healthequity/
For additional OHE fact sheets and information briefs visit: https://www.va.gov/HEALTHEQUITY/Publications_and_Research.asp
REFERENCES
Eliacin, J. et al. (2019). Veterans Affairs providers' beliefs about the contributors to and responsibility for reducing racial and ethnic health care disparities. Health Equity. Retrieved from https://bit.ly/39wVNwh
DeAngelis, T. (2019). How does implicit bias by physicians affect patients' health care? American Psychological Association. Retrieved from https://www.apa.org/monitor/2019/03/ce-corner
The EveryONE Project. (2018). Addressing social determinants of health in primary care. American Academy of Family Physicians. Retrieved from https://bit.ly/36FulLq
IHI Multimedia Team. (2017). How to reduce implicit bias. Institute for Healthcare Improvement. Retrieved from https://bit.ly/2TrGeAm



















