Trends in Coronavirus in Rural Areas
Trends in Coronavirus in Rural Areas: Implications for Veterans
|
 |
SUMMARY
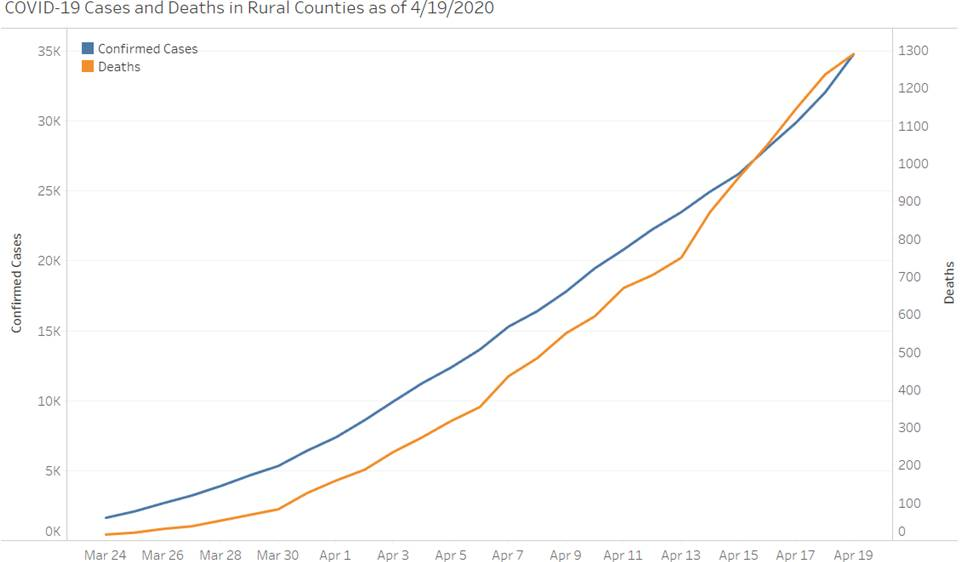
Analyses of data compiled by the Johns Hopkins CSSE 2019 Novel Coronavirus COVID-19 Data Repository show that numbers of COVID-19 cases and deaths in rural counties increased from March 24 to April 19 at a rate faster than in urban counties.
INTRODUCTION
Equitable access to high-quality care for all Veterans is a major tenet of the VA healthcare mission. VA champions the elimination of health disparities, including addressing social determinants of health to achieve health equity for all Veterans. Coronavirus (COVID-19) is a respiratory illness that can spread from person to person. People at higher risk for infection are those who live in or have recently been in an area with ongoing spread of COVID-19.
WHERE VETERANS LIVE AND CORONAVIRUS DISEASE
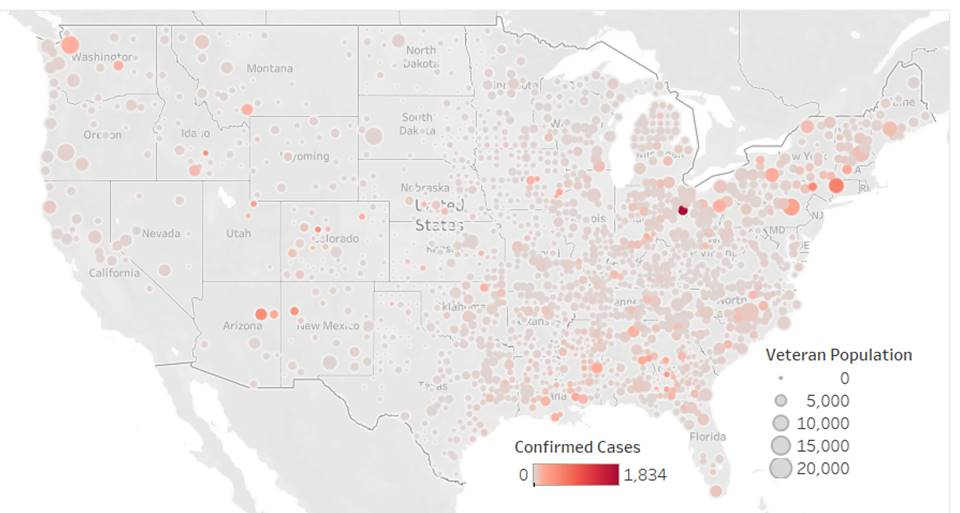
Veterans are more likely to live in less populated areas. Analyses of data compiled by the Johns Hopkins CSSE 2019 Novel Coronavirus COVID-19 Data Repository indicate that numbers of COVID-19 cases in rural counties increased over 21-fold from 1,625 on March 24 to 34,804 on April 19, a rate faster than in urban counties, which increased 14-fold. Also, COVID-19 deaths in rural counties increased over 80-fold; in urban counties deaths increased 66-fold. It is possible that delayed testing rates in rural areas may have contributed to this significantly high rate of cases in rural areas.
VA'S COVID-19 RESPONSE - FOCUS ON RURAL VETERANS
Source: Johns Hopkins CSSE 2019 Novel Coronavirus COVID-19 Data Repository, as of 4/19/2020, CDC Wonder, National Center for Veterans Analysis and Statistics Veteran Population Estimates.
- To access an interactive version of the above data visualization, click here.
- For data on COVID-19 and city Veterans, click here.
Veterans who are at higher risk of severe illness should make sure they have access to several weeks of medications and supplies and establish ways to contact their health care providers, such as using VA Video Connect, in case they need to stay home. Those at higher risk include those 65 years and older, those with asthma, chronic lung disease, serious heart conditions, severe obesity, diabetes, liver disease, or HIV, and those who are immunocompromised or on dialysis.
To get answers to questions about coronavirus and how VA is responding, visit VA’s Coronavirus FAQs page or read VA's public health response. If you have symptoms of fever, cough, and shortness of breath, call your VA medical center before going to a clinic, urgent care center, or emergency room. Calling first helps us protect you, medical staff, and other patients. Alternatively, Veterans can sign into My HealtheVet to send a secure message to VA or use telehealth options to explain their condition and receive a prompt diagnosis. To learn more about what Veterans should do to protect themselves or if they are sick, go to https://www.publichealth.va.gov/n-coronavirus/.
For the latest information about coronavirus, visit the Centers for Disease Control (CDC). For more information about the VA Office of Health Equity visit: https://www.va.gov/healthequity/.
For additional OHE information briefs and fact sheets visit: https://www.va.gov/HEALTHEQUITY/Publications_and_Research.asp
REFERENCES
Centers for Disease Control and Prevention. “What you need to know about coronavirus disease 2019 (COVID-19) Sheet.” https://www.cdc.gov/coronavirus/2019-ncov/downloads/2019-ncov-factsheet.pdf.