Office of Health Equity
Ensuring Rural Veterans Have Access to Care and Research
Ensuring Rural Veterans Have Access to Care & ResearchLauren Korshak, DHealth(c), MS, RCEP, Office of Health Equity, Sarah Gordon, PhD, MS, Partnered Evidence-Based Policy Resource Center (PEPReC), Boston VA Healthcare System, Kelty Fehling, MPH, Denver Center of Innovation for Veteran Centered and Value Driven Care (COIN), Amber Lane, BS, Denver COIN |
 |
We would like to extend a special thanks to the Office of Rural Health and the Veterans Rural Health Resource Center (VRHRC) for their assistance in the development of this brief.
Download PDF
INTRODUCTION
The Veterans Health Administration (VHA) serves a Veteran population that is increasingly diverse. Equitable access to high-quality care for all Veterans is a major tenet of the VA healthcare mission. The Office of Health Equity (OHE) champions the elimination of health disparities and achieving health equity for all Veterans.
HEALTH DISPARITIES
In 2014, Congress expanded the VA’s capacity to purchase health care services for VA enrollees from community providers through the passage of the Veterans Access, Choice, and Accountability Act. Community-based primary care (CBPC) is likely to continue to grow under the 2018 Maintaining Internal Systems and Strengthening Integrated Outside Networks (MISSION) Act’s further expansion of community care.
VA Researchers used VA electronic medical record data from calendar years (CY) 2015-2018 to identify utilization of primary care within VA facilities and CBPC services. The study sample included 7,145,400 Veterans in 3,132 counties across the United States.
They found that CBPC as a proportion of all VA-purchased primary care was small but increased nearly three-fold between 2015-2018. Veterans in rural counties and counties without a VA facility were more likely to utilize CBPC, suggesting that community care may enhance primary care access in rural areas with less VA presence. These findings suggest that offering CBPC does not drive Veterans away from VA facilities, but instead grants access to an alternative source of primary care in areas with fewer VA resources.
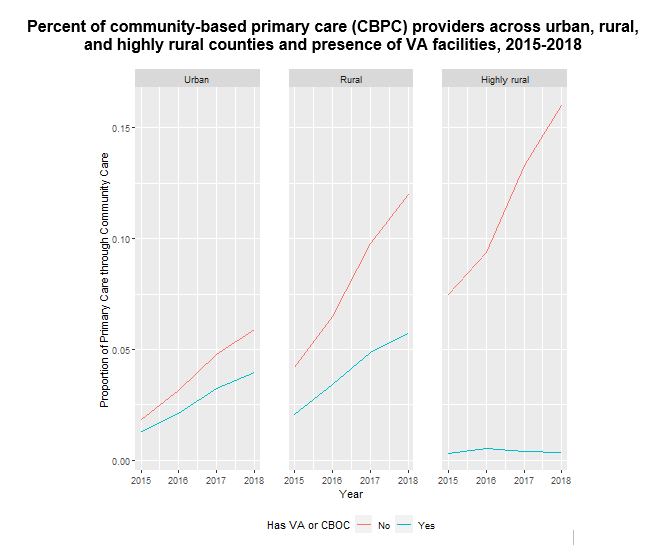
SOURCE: Gordon et al. 2021.
REDUCING DISPARITIES AND IMPROVING ACCESS
The Office of Health Equity supports efforts across VA working to reduce health disparities by targeting interventions aimed at Veteran groups at higher risk for poor health outcomes. Rural Veterans’ lived experiences and expertise are important contributions to VA research projects.
Provider-focused education and inclusive facility policies are beginning to raise awareness about the unique needs and healthcare disparities facing LGB Veterans. There is growing support that these methods have contributed to improved LGB Veteran experience with VHA services.
GROWING RURAL OUTREACH THROUGH VETERAN ENGAGEMENT (GROVE)
In 2020, the Office of Rural Health’s (ORH) Veterans Rural Health Resource Center (VRHRC) in Portland, Oregon funded the Growing Rural Outreach through Veteran Engagement (GROVE) grant. GROVE is a group of VA researchers and Veterans who are located around the country. It serves as a Veteran Engagement (VE) resource center for active research projects whose investigators are interested in engaging in Veteran Engagement as a part of the research projects.
GROVE develops and tests rural VE practices and tools to create best practices around how to best engage rural Veterans in research. GROVE then disseminates these best practices across VA.
GROVE’s Strengthening Excellence in Research through Veteran Engagement (SERVE) Toolkit is updated on an ongoing basis with new tools, templates, and processes for how to engage rural Veterans in VA research projects. The SERVE Toolkit is hosted by the Health Services Research and Development Service (HSR&D) and the Center for Information Dissemination and Education Resources (CIDER).
To learn more about GROVE’s work or request a consultation please contact GROVE Center co-leads Kelty Fehling or Leah Wendleton (Kelty.Fehling@va.gov, Leah.Wendleton@va.gov) or GROVE Center Project Manager Ray Facundo (Raymond.facundo@va.gov).

The Strengthening Excellence in Research through Veteran Engagement (SERVE) Toolkit is found here: https://www.hsrd.research.va.gov/for_researchers/serve/
For more information about the Office of Health Equity visit: https://www.va.gov/healthequity/
References
Gordon, S., et al. 2021. County-Level Predictors of Growth in Community-Based Primary Care Use among Veterans. Medical Care. Jun 1;59 (Suppl3):S301-S306.



















